The use of advanced IT technologies in healthcare opens up new opportunities to improve patient–doctor interactions, enhance treatment quality, and access medical data. Despite the benefits telehealth practices can bring, there exist certain barriers to telehealth implementation. Read on to learn what hinders the adoption of telehealth and find out potential ways to overcome those difficulties.
A US patient consumer survey by researchers from Jones Lang LaSalle (JLL) shows that telehealth is still on the rise. Although the highest demand for virtual visits was during the peak of the pandemic and the number of telehealth visits has significantly dropped since then, the adoption of virtual care among patients remains higher than it was before the COVID-19 outbreak.
Let’s have a look at the most significant advantages telehealth practices can bring.
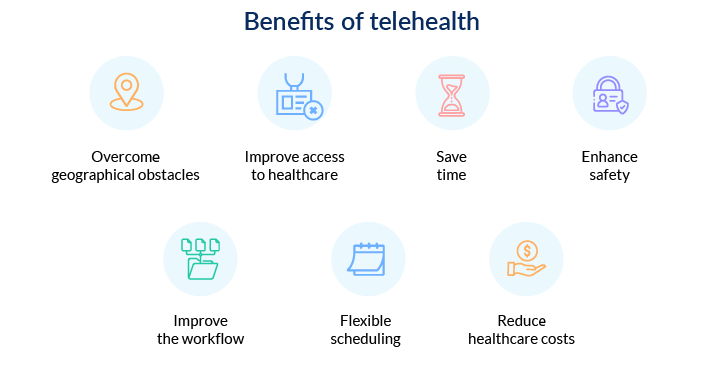
Benefits of telehealth
- Overcome geographical obstacles. Telehealth solutions allow people to deliver and receive quality healthcare regardless of where they are. Additionally, telehealth allows patients to keep their doctor when they move and access care when they live in rural areas with poor access to medical facilities.
- Improve access to healthcare. Clinicians can deliver care remotely, which is crucial for patients who can’t access or experience difficulties accessing a medical facility for any number of reasons. Telehealth may be especially beneficial for elderly patients, disabled patients, or people who simply have no opportunity for an in-person visit.
- Save time. Telehealth solutions can considerably minimize wait and travel times.
- Enhance safety. People with pre-existing conditions or immunocompromised patients are put at additional risk of infection when visiting a doctor in person. Telehealth services are a perfect option for them to receive medical assistance while staying safe at home. Besides, contactless communication with patients enables doctors to stay healthier too.
- Improve the workflow. Video chats take less time than in-person consultations, allowing providers to deliver medical care faster and more efficiently.
- Flexible scheduling. Telehealth solutions can be used at any time and from anywhere, allowing practices to provide extended working hours and weekend assistance with no need to staff a medical facility.
- Reduce healthcare costs. In-hospital healthcare delivery requires lots of resources and therefore is expensive. Telehealth is a good way to reduce costs when there’s no acute need for an in-person visit, such as for a sore throat, pink eye, flu, cough, rashes, etc.
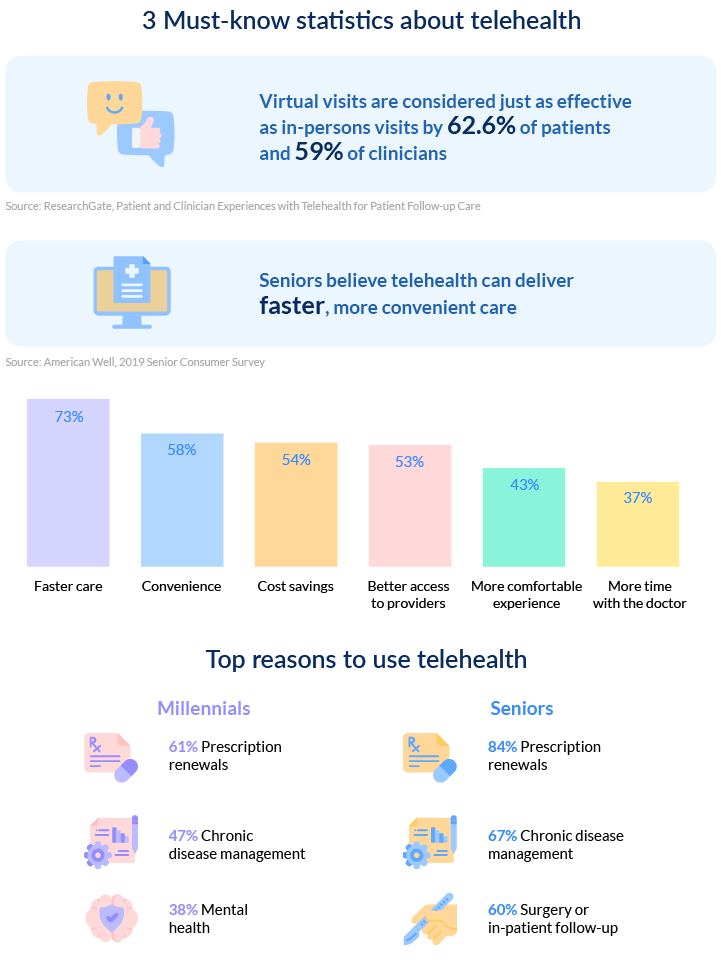
The convenience and ease of telehealth solutions became apparent in light of COVID-19 lockdowns. However, there still exist barriers to telehealth implementation. They can roughly be divided into five categories: behavioral, regulatory, financial, technological, and security. Let’s consider each of them.
Telehealth implementation: Barriers and potential solutions
Behavioral barriers
The new model of delivering medical care still faces a certain skepticism from both doctors and patients. As reported in Deloitte’s Survey of US Physicians, the most significant patient concerns are fear of losing connection with doctors, uncertainty about receiving high-quality medical assistance, and doubts about access issues. Healthcare providers are mostly worried about medical errors that might arise as a result of virtual consultations, patient data security, and access to proper technologies.

Solution
A possible way to overcome this problem is to educate both patients and providers in order to raise their awareness of how telehealth services work, what benefits they can offer, and what to anticipate during virtual meetings. This will allow for cultivating trust, eliminating skepticism, and therefore fostering adoption. The results of surveys and pilot programs, as well as current statistics provided by accredited healthcare institutions, should be publicly available.
As mentioned above, one of the top concerns of healthcare providers is access to proper telehealth solutions. Providers aren’t familiar with the software implementation process. Healthcare experts believe they’ll need to go through a complicated and time-consuming process of installing software and turn to a tech specialist for support.
However, there are telehealth solutions that require no installation and offer two options for medical facilities: to use the software as an independent SaaS product or as a white-label solution. When purchasing a white-label solution, a healthcare provider can rebrand it.
White-labeling has several advantages, including increased patient trust (as patients aren’t worried about using a third-party service, which is critical in terms of telehealth) and no need to spend time and money on creating new software and tailoring it to one’s needs. Purchasing a white-label product is more suitable for large medical facilities, while a SaaS solution will work perfectly for smaller healthcare practices.
Regulatory barriers
State regulatory bodies and legislatures are crucial contributors to telehealth policies. These policies vary across the states, and legal restrictions are one of the biggest obstacles to telehealth implementation. Regulatory barriers can be categorized as follows.
- Reimbursement. Low reimbursement is considered a significant disincentive. According to American Well’s survey, 77 percent of healthcare providers view lack of reimbursement as the biggest telehealth challenge. A report by the University of Michigan’s IHPI says that telehealth is compensated in limited circumstances. Moreover, there still exists a payment disparity between regular office visits and telehealth care. In some states, offline and online visits should be charged similarly, while in others, this issue is left to the insurer’s discretion. However, major US health institutions are trying to address these problems. For instance, CMS has offered to include telehealth services in the basic Medicare Advantage plan in 2020. Previously, CMS compensated telehealth services for rural beneficiaries with restricted access to traditional medical units.
- Licensing. Licensing requirements are different across the US. Typically, clinicians are required to obtain a license in the state in which they work. However, some states issue special telehealth-related licenses and certificates. Such permissions allow out-of-state providers to render telehealth services in states they aren’t located in or if specific requirements are satisfied (e.g. agreements to not open offices in the chosen state). The problem of licensing causes increased overhead costs for clinicians and significantly slows down telehealth adoption.
- Credentialing. This is another deterrent and demotivating factor in the process of telehealth adoption. Clinicians are supposed to have telehealth credentials at every hospital they work according to the hub-and-spoke model. The process is rather complicated, and the costs affiliated with it are burdensome.
- Malpractice liability is another one of the top barriers to telehealth implementation. So far, there have been few telehealth-related malpractice cases, with many of them revolving around teleradiology. However, this is associated with the laggard adoption process. Theoretically, the number of such cases is likely to grow as telehealth solutions grow in popularity. There’s a crucial issue practitioners should be aware of, and that’s malpractice coverage.
Solution
Potential ways to overcome the regulatory barriers mentioned above are:
- Bringing in new, transparent, and uniform reimbursement models that will be applicable across the US is crucial to stimulate telehealth adoption.
- Providing licensure agreements allowing clinicians to deliver telehealth services outside the licensed area and working in other states without extra licenses are possible solutions to the problem.
- Elaborating a standard requirement set to simplify the credentialing process would allow practitioners to apply for credentials at several hospitals in one go. The initiative by the CMS supports delegated credentialing, or credentialing by proxy (CBP). This means that if a clinician is already credentialed at a Medicare-supported healthcare facility, it should be sufficient for rendering telehealth services at another facility.
- Making sure that healthcare providers’ malpractice insurance will be viable in the states in which they deliver care.
Financial barriers
Funding remains one of the biggest barriers to implementing telehealth. Upfront costs such as investments in purchasing and installing specific equipment, establishing and supporting the network, and obtaining the required dedicated technical skills are overwhelming. Besides, there are many other recurring accompanying expenses, such as paying for electricity and internet, support team salaries, etc.
Solution
To motivate clinicians and accelerate the adoption of telehealth services, pay-for-performance (P4P) schemes can be implemented. Such schemes nudge providers towards rendering value-based services and align payment with quality and patient satisfaction. It would help if governments gave preference to multilateral funding and public-private partnerships. This would guarantee the cost-effectiveness and sustainable development of telehealth programs and spread the initial cost loading.
Technology barriers
Uncertainty about technology and lack of knowledge to leverage it are major barriers to telehealth implementation. Healthcare providers aren’t aware of what technical solutions are on the market, how these solutions can help them with their workflow, and how they can benefit from using telehealth services. Besides, there’s a lack of trust and confidence in the outcomes of telehealth care. These facts significantly slow down the overall growth of the telehealth sector.
Solution
Governments should allocate funds for offering practical training to healthcare providers on modern telehealth technologies to make them more familiar with and confident in using telehealth for care delivery. Doctors are key contact points for their patients. So they will have the power to convince people to solve their health issues via telehealth services.
Security barriers
Another important issue that worries both patients and doctors is medical data privacy and security. Telehealth users often have questions about HIPAA compliance. There are no specific requirements for telehealth services. However, as remote care delivery entails installing specific software for virtual consultations, this software must meet all HIPAA security requirements. Also, providers should be aware of any additional security-related laws of the states in which they work.
Solution
Healthcare providers should consider integrating modern telehealth solutions that are HIPAA-compliant and can provide seamless virtual visits. For example, services like Skype can’t be leveraged, as they don’t meet HIPAA requirements.
The bottom line
To sum it up, there are multiple barriers to implementing telehealth solutions. However, the growing popularity of telehealth services and the awareness of how telehealth can change the whole healthcare system globally will finally accelerate the process of its adoption. It’s high time to find a reliable tech partner.
While choosing a proper solution, opt for HIPAA-compliant, secure, multi-functional, and high-quality meeting software to take maximum advantage of telehealth solutions. Explore our guide to learn how to choose the best telemedicine software for your facility.
FAQ
-
Barriers to telehealth implementation can roughly be divided into five categories:
- Behavioral
- Regulatory
- Financial
- Technological
- Security



