Before their first telemedicine appointment, you should equip patients with necessary knowledge and resources and demonstrate how easy, convenient, and continuous virtual medical care can be. Patients can get the same quality of care via telemedicine video consultations as they would get with in-person visits, all without sitting in a waiting room. You'll improve patient satisfaction, which will affect your telemedicine practice's growth.
In this article, you’ll find nine helpful tips to prepare patients for their first experience with telemedicine.
1. Explain informed consent
Prior to the first telemedicine visit, healthcare providers must receive permission from patients. Make sure you communicate to the patient:
- what technology you’ll be using
- who you’ll contact (and under what circumstances) in case of any issues from the patient’s side. This might be a friend, family member, or other healthcare provider
- all services and procedures you’re going to provide
- privacy and security of virtual healthcare services
- patient rights and responsibilities during telehealth visits. You might ask patients to wear headphones, find a private space, or double-check with their health insurer regarding telehealth coverage
Furthermore, you can create a legal agreement and send it to patients by email once they book an appointment.
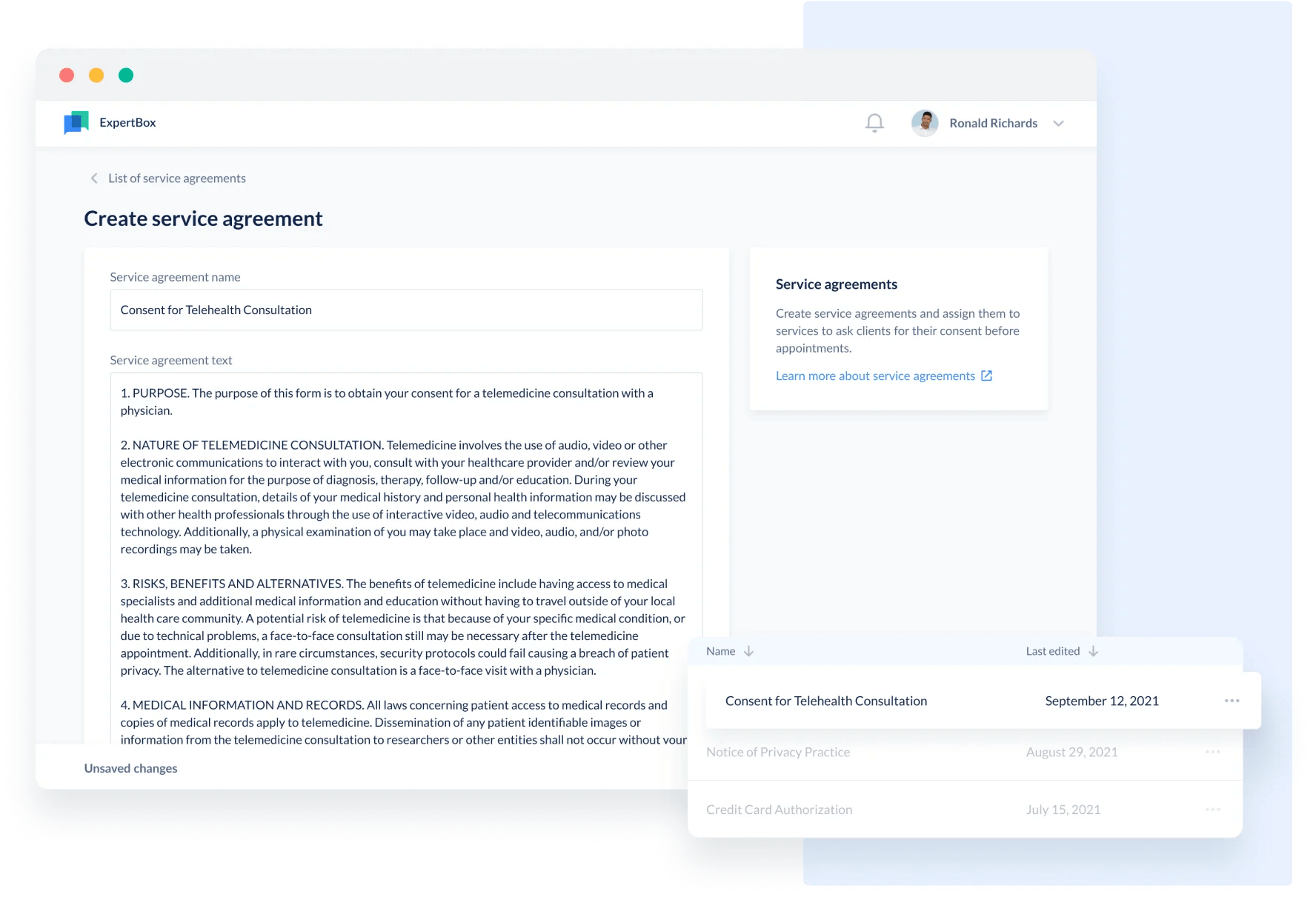
Sending legal agreements at the point of booking a visit is the simplest and most cost-effective approach. In doing this, healthcare providers can comply with industry-specific requirements and not waste time on documents during the visit.
Create legal documents, share them with patients, and see how easily it can be done with ExpertBox service agreements.
2. Highlight telemedicine benefits and patient responsibilities during virtual care
Illustrate telehealth advantages to patients and explain how these advantages outweigh possible drawbacks. Key telemedicine benefits include:
- increased access to medical care without any loss of service quality
- reduced transportation costs
- time efficiency
- ability to interact with the provider via multiple devices at any convenient time using online booking and appointment scheduling
Additionally, you should inform your patients about telemedicine privacy risks and security considerations. Patients should be responsible for keeping their space private and secure to avoid disclosing health-related information. Ask patients not to share or discuss sensitive information, such as their lab results and diagnoses, with the physician over social networks, messengers, or other software that is not HIPAA-compliant.
Patients might also be concerned about the security of their data. Show your patients that their privacy is your top priority. Using HIPAA-compliant clinic software ensures patients encounter minimal to no privacy and technical constraints. HIPAA-compliant telehealth vendors provide secure video calls, messaging, cloud storage, and data encryption to prevent fraud.
Pro tip: Inform patients of HIPAA requirements in the US and PIPEDA in Canada. Apart from HIPAA, some US states may have additional telehealth requirements.
These aren’t the only ways remote healthcare improves patients’ satisfaction. Explore 11 compelling benefits of telemedicine for patients and what stands behind each of them.
3. Define the limits of your licensure across state lines
When the pandemic began, Medicare and Medicaid temporarily modified rules that required healthcare providers to be licensed in the state where the patient is located. Today, many states have rolled back temporary pandemic workarounds, so healthcare providers can’t simply practice remote care everywhere.
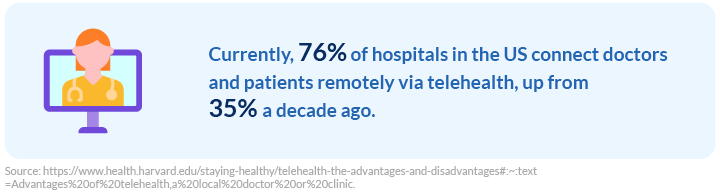
Make patients aware of which state you’re licensed in and ask if they plan to have an appointment with you in another state. You can also develop alternative coverage plans when a patient is out of your jurisdiction.
4. Outline your documentation policies
Augment your documentation policies and procedures to ensure the privacy and security of protected health information (PHI). Consider the following aspects:
- what extra documentation you must keep for telehealth visits
- how you document patient health records (paper, EHR, locked file)
- who else can view your notes and documents (nurses, office staff, other medical professionals)
5. Discuss your policies if you lose your laptop, cell phone, or tablet
If your device is lost or stolen, you must contact each of your patients in writing, as this might lead to the loss of patient data and risks such as identity theft. Let patients know a breach has happened as well as the actions you’re taking to protect their information from unauthorized access. For example, you can remotely erase data on your lost or stolen device. Also, you might report your missing device to the Office of Civil Rights in the United States (or other entities in foreign countries).
6. Do a technology check
To provide a quality telemedicine experience, review potential technology pitfalls before initiating the first telemedicine visit. Furthermore, consider checking:
- adequacy of bandwidth to avoid connection issues
- reliability of telehealth equipment (computers, laptops, headphones, microphones)
- camera resolution, room lighting, and microphone placement
You should learn and master your technology and train with medical staff and colleagues for at least several hours to gain confidence in using the software. During your first set-up session, create a plan on how to solve possible patient issues such as video or sound problems, dropped connections, etc. When patients visualize the overall telemedicine visit process, they will be more willing to use telemedicine.
Learn how to help medical staff seamlessly implement telemedicine step by step.
7. Create an emergency plan
Patients should be prepared for emergencies, especially when they are outside the clinic’s control. An emergency might occur from various causes, including a change in mental state, heart attack, overdose, breathing problem, etc. Confirm the following during the first appointment:
- the patient’s exact location and full address.
- emergency numbers for the patient’s location. 911 works if you and your patient are in the same area.
- who the local emergency contact or support person is to offer help in a crisis. This might be a family member, neighbor, or close friend.
- alternative ways to reconnect with the patient if the connection drops or doesn’t function properly.
8. Discuss with patients how to minimize interruptions in their home environment
Help patients set up their first telemedicine visit and prepare for possible interruptions such as phone calls, children needing attention, a family member unexpectedly entering the room, or the doorbell ringing. Ask patients beforehand to eliminate any background noise and not allow other people to enter the room to maintain privacy.
9. Develop policies about charging for missed appointments
Patients miss appointments due to many factors, including financial and scheduling issues.

Before the first telemedicine visit, educate patients regarding appointment scheduling policies, including rescheduling and cancellation rules. Add a no-show policy to your informed consent agreement. When patients are informed about extra fees when they do not show up to their appointment, they will be inclined to reschedule instead of simply not showing up. This will help reduce patient no-shows and prevent you from losing revenue.
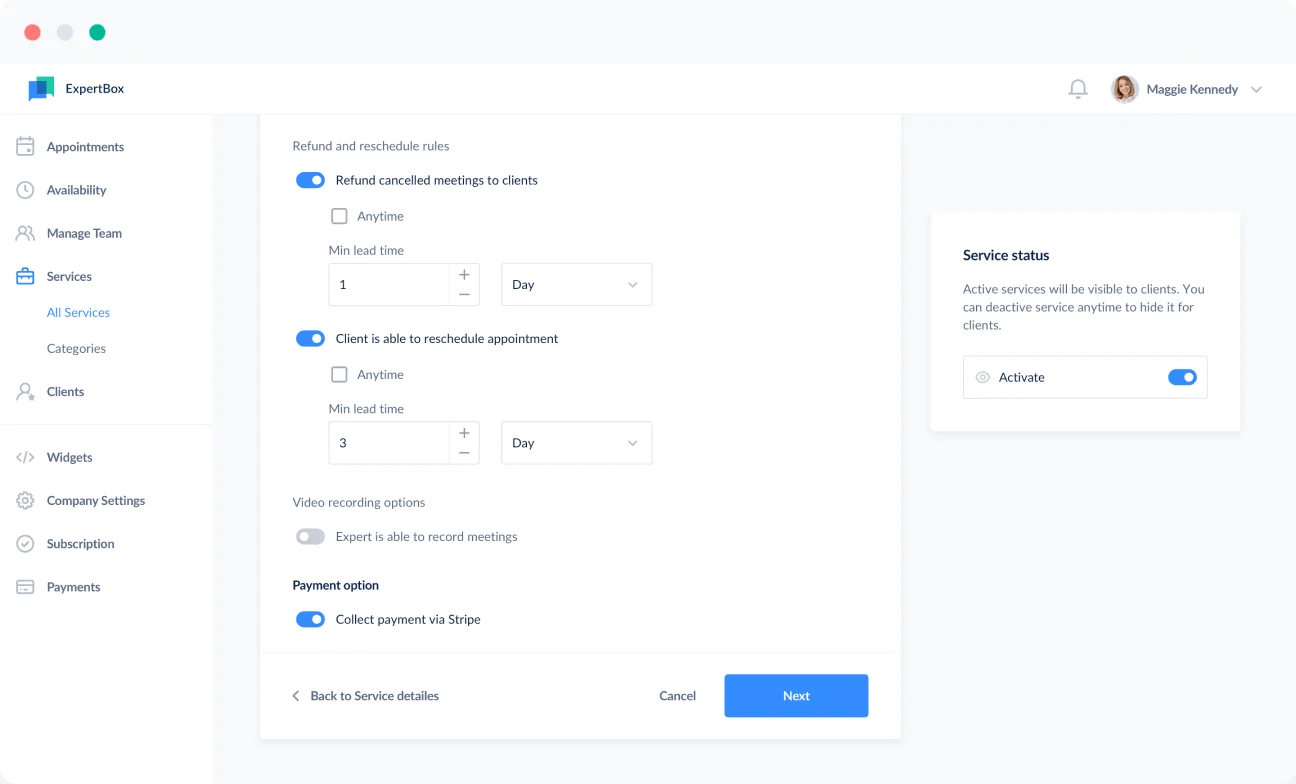
Advanced telemedicine platforms like ExpertBox allow healthcare providers to set refund and rescheduling rules for telemedicine services. This means you get paid 100% of the time, even if appointments are unexpectedly canceled.
Automated reminders have also proven effective for patients who tend to miss or forget about upcoming appointments. Scheduling and online booking let patients be in control of their own time. Patients can book an empty slot on a provider’s calendar that best suits their schedule.
Summing up
The key to effectively preparing your patients for telemedicine is to put yourself in your patients’ shoes and truly understand their desires, worries, and other emotions. This ensures patients’ comfort and safety during telemedicine visits and allows you to maintain quality care. With good preparation, there’s no reason remote care cannot be as successful and efficient as in-person appointments.
Subscribe to our blog to be the first to learn about telemedicine best practices.
FAQ
-
#1 Explain informed consent
#2 Reveal telemedicine benefits and patients’ responsibilities during virtual care
#3 Define the limits of your licensure across state lines
#4 Outline your documentation policies
#5 Create policies in case you lose your laptop, cell phone, or tablet
#6 Develop a solid plan to deal with technical problems
#7 Manage patients who contact you from outside your licensed jurisdiction
#8 Make agreements with patients to minimize interruptions from their home environments
#9 Develop policies about charging for missed appointments



