Telehealth technology promises to improve patient outcomes and increase physician efficiency. Seeing its great potential, 84 percent of healthcare executives started embracing telehealth around 2014. Since then, early adopters have successfully overcome numerous telehealth challenges and paved the way to widespread adoption of this technology.
Although telehealth is becoming more approachable, however, practitioners still have a few barriers to remove. What are the challenges of telehealth? In this article, we talk about the common challenges you might face when starting to implement telemedicine and effective ways to cope with them.
#1 Lack of trust in telehealth services
The Deloitte 2016 Survey of US Health Care Consumers revealed that 43 percent of respondents thought the care provided through telehealth services would be substandard. People thought that during virtual visits, physicians wouldn’t be able to access the same level of information about patients’ well-being as they can during in-person physical exams. Still, people showed a willingness to try different telehealth options.
Two years later, the Deloitte 2018 Health Care Consumer Survey reported 77 percent satisfaction among patients who had tried virtual visits. Respondents admitted that virtual appointments were more convenient, required shorter wait times, and cost less. Nevertheless, the survey showed that only 53 percent of patients said the practitioners they saw online were as professional or knowledgeable as someone they would see in person.
Tips to build trust with your patients
- Ask your patients their opinions about telehealth to know what concerns you should address and what incentives you should offer to encourage them to use telehealth services.
- Share information about research and surveys that show the benefits and prove the effectiveness of telemedicine services.
- Collect testimonials from your satisfied patients to convince others about the high quality of your telehealth service.
#2 Fear of data compromise
The general public is impressed (and not in a good way) by the number and scale of recent cyber attacks in the healthcare sector. This feeds their second-largest telehealth-related concern about information security and makes them think that remote care technologies are vulnerable and represent a potential threat.
Healthcare providers should meet security requirements and ensure the HIPAA compliance of telehealth services, which narrows their choice of software. Software vendors are aware of this problem and respond by investing in cutting-edge security technologies including data encryption, access controls, and blockchain solutions. Aftrex Market Research predicts that the market for blockchain technologies in healthcare will reach $5,517.6 million by 2026 because this technology has proven a good option for safe data management, billing, and claims settlement.
Tips to protect patient information
- Work with telehealth software vendors that implement the latest security technology and can prove their solutions comply with the HIPAA Security Rule.
- Provide your employees with regular HIPAA Compliance Trainings to be on top of recent changes in legislation and comply with the HIPAA Privacy Rule.
- Dispel fears by proactively communicating how you take all necessary measures to protect your patients’ personal information.
#3 Difficulties with implementation
Resistance to change is a common telehealth challenge practices face when they want to add remote care services. Introducing telemedicine will require you to make significant tweaks to existing workflows and invest time and effort in training your employees.
When introducing telehealth to your practice, you should get buy-in from your colleagues. For this, you should explain to your team what pain points telemedicine will eliminate. Some team members may be motivated by the prospect of having less exposure to illnesses, while others may value automated appointment management the most. Once you gain the support of your team, provide them with technical information and training to ensure a seamless start.
Tips to streamline implementation of a telemedicine system
- Choose software that provides great usability and customer support to make using telehealth services simple for both patients and caregivers.
- Look to the American Telehealth Association (ATA) or similar organizations for information on telehealth best practices, case studies, and implementation examples.
- Provide training for your colleagues and incentivize practitioners who engage in telehealth to decrease their resistance to adopting this technology.
#4 Cost of adding telehealth services
The cost of special equipment for telehealth may be high, which may deter you from investing in this new line of service. However, in most cases, remote care requires a physician to have nothing but a computer and a headset.
Case studies prove that telehealth is worth the investment and reduces healthcare providers’ costs in the long run. For example, Intermountain Healthcare hospitals managed to save up to $137 per episode of care after they launched their Connect Care telehealth service. You can learn how remote care helped other healthcare providers save money and estimate how much you can save by following their approach.
Tips to reduce telehealth costs
- Look at online resources to get a better idea of how much it may cost you to start a telemedicine product and what expenses you should expect.
- Assess the technical needs of your telehealth program before purchasing any equipment or software to avoid wasting money on things that are too sophisticated for your needs.
- Research the software available on the market and try out several options to make an informed purchasing decision.
#5 Reimbursement uncertainty
Every state has its own policies on coverage and reimbursement for telehealth services, and these policies continue to change. Today, 42 US states have laws that govern private payer reimbursement for telehealth services. However, it’s important to note that not all of them mandate reimbursement parity between in-person and virtual care. Coverage of telehealth services by Medicare and Medicaid insurance programs also varies by state. This uncertainty frustrates providers and complicates the implementation of telehealth services.
All the same, telehealth reimbursement policies across the US are improving with time. Medicare and Medicaid as well as private health plans continue to expand their coverage of telehealth. Apart from that, patients show a strong willingness to pay out of pocket for timely diagnosis and treatment to avoid missing work, having to find childcare, and having to drive to a clinic.
Tips to improve your return on investment
- Pay close attention to changes in laws and regulations in the states in which you operate to avoid liability issues and capture emerging opportunities.
- Track updates from the Centers for Medicare and Medicaid Services (CMS) and private payers to know the correct telemedicine billing codes.
- Give patients clear guidance about what services their insurance covers and what services they should pay for out of pocket.
Despite all the telehealth challenges, McKinsey projects that the telehealth market may grow to $250 billion in the near future. Providers who’ve already started rebuilding their care delivery models and investing in remote care will be the first to get their share of this revenue. It’s time to act! Look at the infographic below to see what opportunities telehealth offers for your medical practice.
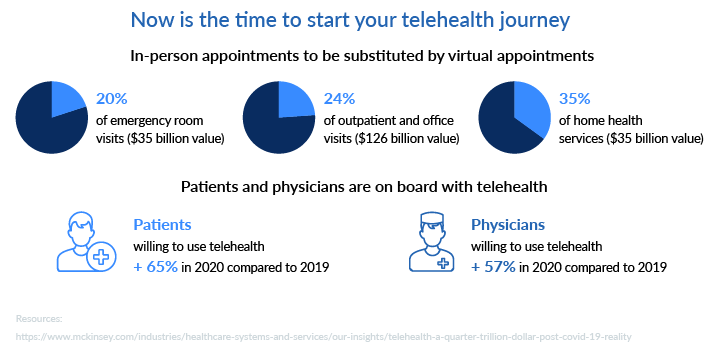
The simplest way to get started with telehealth
There’s no doubt that starting a telehealth program will bring new challenges. However, you have no reason to lose out on this opportunity. Armed with cutting-edge technology, progressive care delivery methods, and industry best practices, your business will thrive through change.
If you’re still hesitant about introducing telehealth in your practice, start small by taking a look at our handy guide to getting started with telemedicine that covers opportunities, challenges, and best practices. See how medical appointment scheduling software can streamline your patient care delivery.

