As information technology advanced, telemedicine had been taking new forms and gradually growing until the COVID-19 pandemic brought it into the spotlight. Since the start of the pandemic, healthcare providers who had hesitated to adopt telemedicine have given it a go out of necessity and soon realized its potential.
Now, telemedicine is quickly gaining trust from patients and practitioners and becoming an integral part of the new healthcare delivery system. But despite the growing popularity, there’s still some confusion around what exactly telemedicine is and what it offers. This article will give you a clear idea of the scope of telemedicine, a typical telemedicine workflow, and common use cases.
What is telemedicine
Telemedicine is the practice of providing medical services remotely via real-time interactive communication between patients and healthcare providers with the use of telecommunications technology. Telemedicine can be used to provide three types of medical services to patients: remote patient monitoring (RPM), video conferencing, and store and forward (S&F).
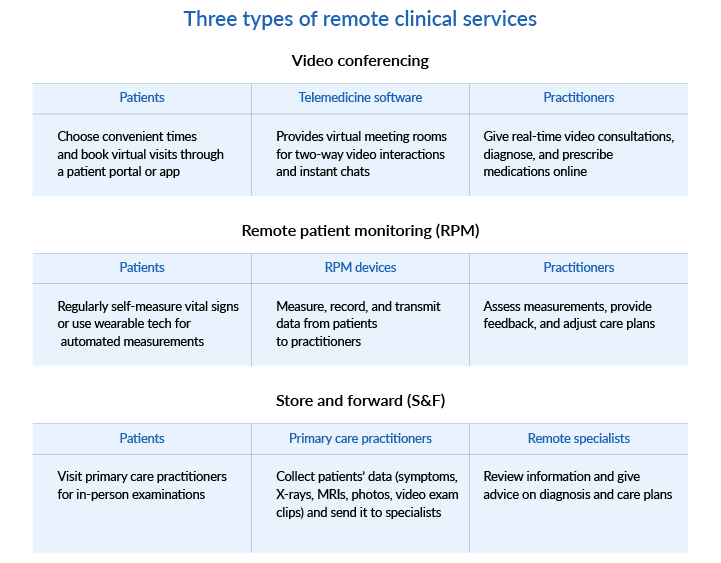
You can use secure telemedicine video conferencing software to communicate with remote patients in real time. If you’d like to implement periodic or continuous monitoring of vital signs for home care or patients with chronic conditions, you should take a closer look at RPM technologies. Store and forward technology will help you collect patient information and share it with specialists in remote medical settings to get their assistance with diagnostics and developing care plans.
Although all three types of service are commonly attributed to telemedicine, sometimes you can see this term being used to mean video conferencing only. The other two services in this case may be attributed to telehealth.
Evolution of telemedicine
Your timeline reaches back less than one century. The technology available at every new stage of its development has shaped its use and accelerated its spread. The timeline below recaps the main milestones in the history of telemedicine from the early 20th century onwards.
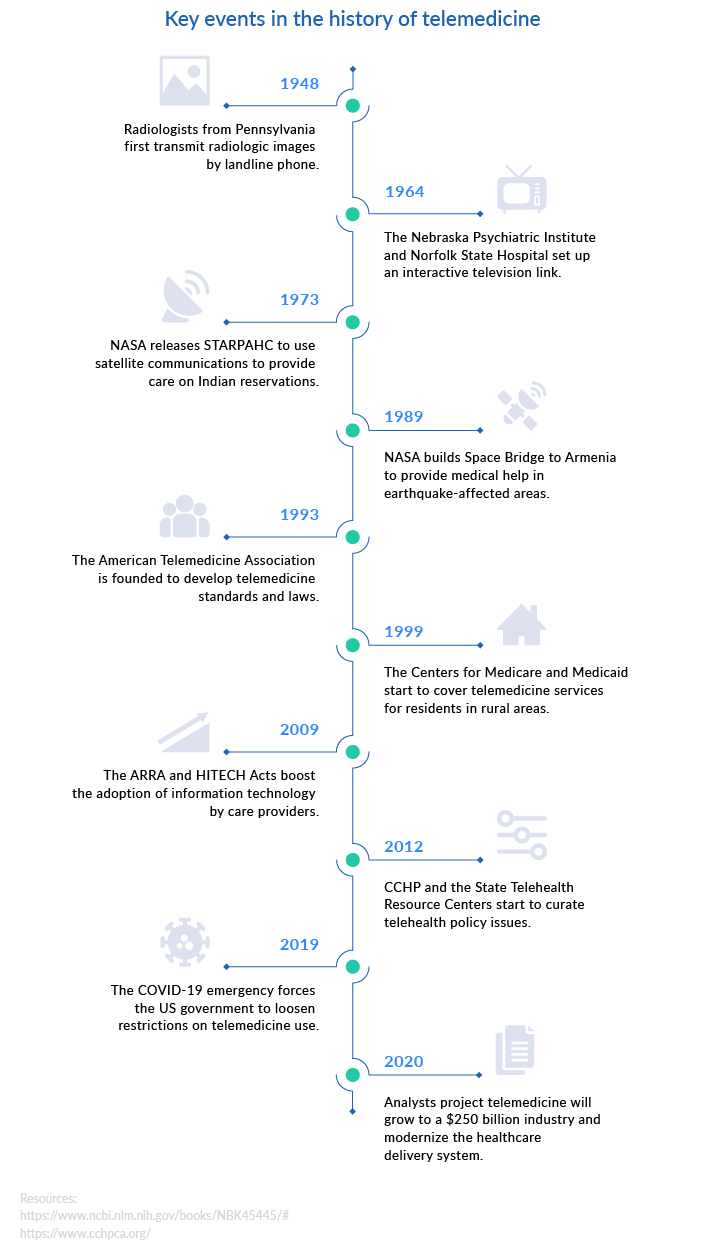
The original goal of telemedicine was to provide medical services to people that lived far away from healthcare providers. Today, the goal has shifted from overcoming distance to offering convenience. As people get accustomed to various online services in entertainment, retail, and education, healthcare providers have to meet rising expectations.
How telemedicine works
So far, telecommunication in the form of video conferences remains the most well-known and most widely used type of telemedicine. It also has the best insurance coverage. And there’s a reason for that. While remote patient monitoring and store and forward are used to strengthen personal visits, video conferencing is used to replace them. It streamlines patient–practitioner interactions and allows caregivers to communicate with patients who are in different cities and states, providing the same or even a better quality of care compared to in-person visits. So how does telemedicine work? Let’s look in detail at how healthcare providers use virtual visits.
Scope of virtual visits
Virtual visits are of great help when patients have minor health issues that don’t require lab tests or imaging to make a diagnosis and prescribe treatment. Another popular use of video conferencing is for follow-up care that requires quick check-ins. Consider offering your patients to substitute in-person visits with virtual visits in the following contexts:
- Post-treatment follow-ups. Touch base with post-discharge patients to check if everything is fine without bothering them to travel to your office.
- Check-ins for patients with chronic conditions. Reduce the number of regular in-person visits for patients with chronic conditions and adjust their care plans remotely.
- Refill prescriptions. Help your patients with urgent short-term refills of their regular medications that are not considered controlled substances.
- Minor urgent care. Inform your patients about minor health issues for which they can seek remote urgent care instead of going to an emergency room.
- Nighttime care. Provide after-hours virtual care to patients who can’t wait until the next morning to schedule an in-person visit.
- Lab/imaging results review. Discuss patients’ abnormal lab results face to face during a video call to present information clearly and in a timely manner.
- Serving distant areas. Improve continuity of care for patients who live in distant areas and can’t travel to your office every time they need care.
- Treating people with mobility issues. Make care more accessible to elderly people or people who have difficulties with mobility.
- Travel care. Allow your patients to access your care when they’re on vacation or on a business trip instead of looking for a local doctor with whom they’re unfamiliar.
The scope of telemedicine services you’ll be able to offer depends on state laws and policies. However, even if you introduce one or two options that will cover a true needs, you can close gaps in care and move your service to the next level.
Virtual visit workflow
Telemedicine brings organizational changes and has its own workflow and best practices. To provide a high standard of service and meet patients’ expectations, you should have clear protocols for before-, during-, and after-visit procedures. Here’s an example of a telemedicine workflow suggested by the American Medical Association that you can adjust and use in your practice.
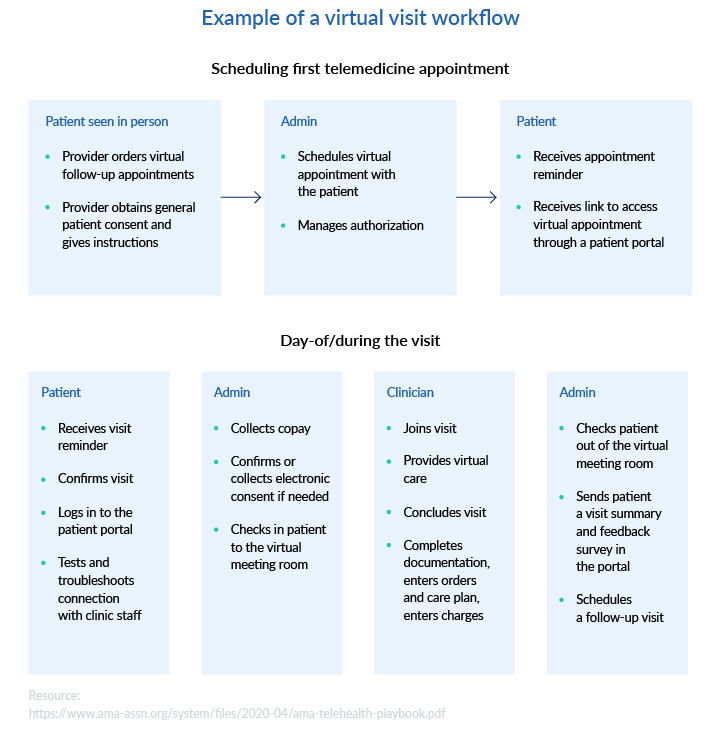
Virtual visit best practices
When introducing telemedicine, you should ensure that patients receive appropriate care that complies with medical standards, state laws, and reimbursement policies. You should also fit virtual appointments into your care team’s workflow in the most efficient way. We suggest you consider the following tips on scheduling, conducting, and documenting your virtual visits to properly set up your new line of service.
Pre-visit tips and advice. Telemedicine works well when booking and scheduling are set up in a way that’s convenient for patients and care team members.
- Find the best time to provide telehealth visits, whether it’s throughout the day, during specific clinic hours, or after hours
- Provide a 5- to 15-minute buffer between virtual visits and decide on lead times for scheduling new appointments to make sure you can keep up with your schedule.
- Set procedures for collecting patient informed consent and set triage protocols for when a telehealth appointment is appropriate.
- Find ways to ensure a match between a patient’s location when they seek care and your ability to provide care in that area according to your medical license.
- Provide convenient ways for rescheduling and cancellations of virtual appointments that would minimize administrative work for you and be convenient for your patients.
- Ensure fast and secure access to virtual meeting rooms via your telemedicine software as well as automatic appointment confirmations and reminders.
During-the-visit protocols and etiquette. Online communication differs from in-person communication. It has its own etiquette and requires practitioners to develop specific technical and communication skills:
- Have a quiet, properly equipped, and well-lit room where you’ll conduct virtual visits in a way that ensures privacy and convenience.
- Set clinical guidance for remote physical exams when applicable and know how to instruct patients to conduct a self-examination.
- Get ready to troubleshoot in case of technical glitches, a bad internet connection, or patients being late to the appointment.
- Ensure you have technology in place to message, share your screen, send files, take notes during online visits, and record your video consultations.
- Practice video conferencing skills to ensure you speak clearly, use non-verbal language, verbalize, clarify the next steps, narrate your actions with patients, etc.
Post-visit musts. Remote interactions with patients should be properly documented and saved using your telemedicine software, EMR, and EHR systems:
- Think about how you’ll organize and save your notes, visit summaries, documents, and video records to keep all of a patient’s health information in one place and accessible.
- Provide some time after the visit to manage care plans and prescriptions for the previous patient and recall information on the next patient.
- Set up procedures for soliciting post-visit feedback from patients via a live chat or survey forms available in your telemedicine software.
- Check a patient’s payments or manage reimbursement billing and paperwork and track the statuses of reimbursement claims.
Once you set up your telemedicine program, make sure to provide your patients with comprehensive information about their new care options and how telemedicine works. You can share lists of appropriate cases in which to use telemedicine, infographics showing benefits for patients, technical FAQs, step-by-step guides explaining what happens during a virtual visit, etc. This will help you set clear expectations and make it easier for patients to opt for virtual care.
Who can use telemedicine
Any healthcare professional can use telemedicine when it’s applicable to specific patient conditions. Telehealth is ideal for first consultations, follow-up visits, and other non-urgent cases that can be handled remotely and don’t require a patient’s physical presence.
How else telehealth can help healthcare providers manage patients’ health and well-being:
- provide annual check-ups
- monitor patient symptoms in real-time
- evaluate lab tests
- adjust treatment plans
- tackle mental health issues and others
Telemedicine vs telehealth
It’s not that easy to determine what the difference is between telemedicine and telehealth because each US state and each organization has its own definitions of telemedicine and telehealth. Moreover, those definitions often overlap or slightly differ. As a result, some healthcare professionals use these terms interchangeably, while others insist they are not synonyms but fail to agree on their definitions.
The most widespread opinion is that telemedicine refers to clinical services only, while telehealth expands beyond such services to include patient portals and medical and health education. The final definition of what telemedicine is and how it relates to other terms from the broad domain of digital health remains a work in progress. Until healthcare professionals reach a common position on it, you can use the chart suggested by C. Milaster to navigate the digital health taxonomy.
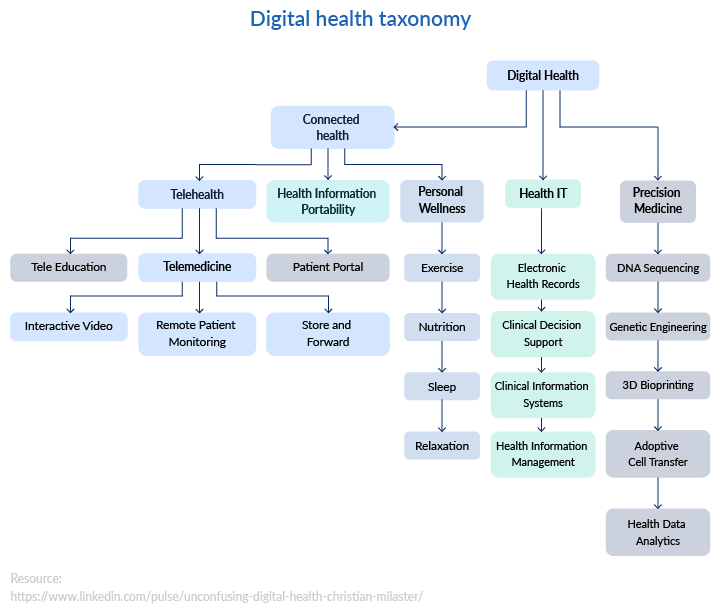
Telemedicine is the future of healthcare
Your own experience with telemedicine can turn into a real success story. If you’re looking for more information on telemedicine, read our Practical Guide to Starting Telemedicine to find out all the benefits, opportunities, and best practices of telemedicine to make even more grounded decisions.



