Many patients have returned to physicians’ offices as society has reopened, but many also appreciate the convenience of telehealth. According to a recent survey by Optum, 90% of patients said their favorite part of telehealth is how convenient it can be. Remote monitoring is deemed a great alternative to traditional in-person visits and, sometimes, the only means for clinicians to consult and treat patients. This makes telehealth a necessity in today’s care delivery. Most patients who used telehealth in 2021 expect to use it again in 2022, while younger generations (digital natives) are likely to continue using telehealth.
Armed with suitable telehealth technology, including for secure video meetings, chat, and online bookings, medical organizations can deliver valuable care whenever patients need it. This article reveals practical tips to make your telehealth visits stand out.
#1 Assess the needs of new and existing patients
Patient–physician relationships remain key to positive health outcomes with both new and established patients. Healthcare providers should evaluate the needs of each patient and decide what type of appointment would be suitable for each specific case — an in-person visit or a virtual one. For example, if an established patient asks for a further consultation, it may be appropriate to consult with them via chat or arrange a call, no matter where they are.
The same goes for setting up first-time appointments. Just because you can arrange the initial visit online doesn’t mean that’s always a good idea. However, it might be a good idea when the patient just needs to describe a symptom and make sure everything is on track or check lab results without going to the clinic. In other cases, especially when a physical examination is necessary, it’s reasonable to meet a patient in person (at least for the first time).
#2 Ensure privacy
According to the 2021 HIMSS Cybersecurity Survey, phishing attacks and ransomware are the most common healthcare security incidents, but phishing remains king. In this survey, 67% of respondents indicated that their healthcare organizations experienced numerous security incidents in the past twelve months.
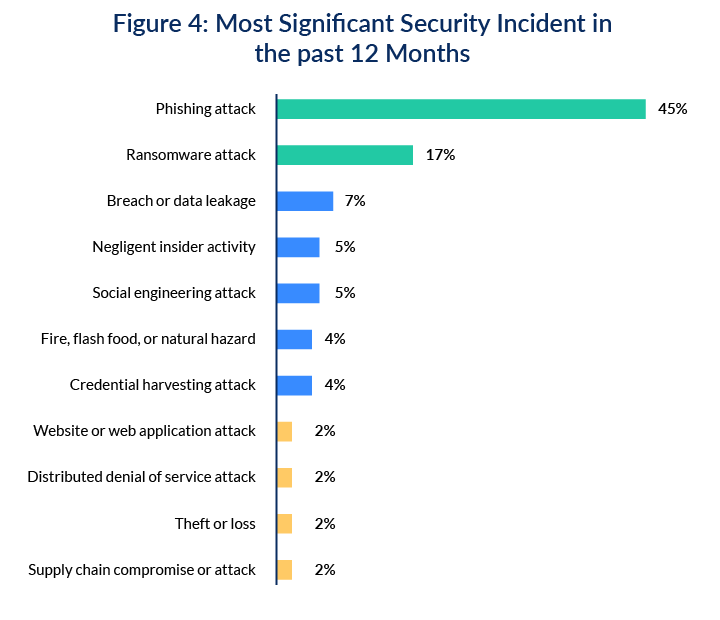
Hackers can send malicious emails to physicians and patients that cause data theft. Such phishing emails can contain links or attachments that can infect clinic software with malware or viruses. If you receive an email that looks suspicious, it’s best to disregard it or delete it from your inbox.
Pro tip: Choosing clinic management software that is HIPAA-compliant (with an end-to-end encryption method and robust authentication) allows clinicians to avoid data breaches and scammers’ attacks to compromise sensitive patient data.
Healthcare providers must ensure any data entrusted by patients is kept private, whether in storage or transit. This allows facilities to increase patient loyalty and avoid the high monetary costs of taking corrective actions over HIPAA noncompliance.

Unsecured communication channels such as SMS, Skype, and email should not be used for communicating ePHI. Only authorized users should access ePHI, monitor it, and delete it remotely if necessary. This serves as the pillar for patient privacy. Providers can communicate with patients only via secure video conferencing and messaging.
#3 Select a telehealth vendor
Telemedicine software can help expand patients’ access to care and simplify care delivery for medical providers. When researching available options, make sure that your chosen technology:
1. Enables clear and seamless communication between patients and providers
Software should be:
- Easy to install, use, and update
- Efficient and reliable
- Intuitive
- Web-based
- Independent of third-party software
2. Meets security standards
Telehealth visits are more vulnerable to privacy and security threats than in-person consultations. Telehealth providers must be responsible for compliance with system security requirements and patient confidentiality. Stored patient data should never be available outside the telehealth system. Choose a telehealth platform for your facility that is encrypted and complies with HIPAA security requirements.
3. Offers a set of features to satisfy all your needs
Make a checklist of what functionality you need, such as online booking, scheduling, chat, team management, reminders, and video conferencing. This way, you prevent yourself from opting for features that might be totally useless once the software is installed.
4. Allows you to save money in the long run
A cost-effective telehealth solution doesn’t mean just being more budget-friendly. The telehealth platform you choose should be an instrument to solve common problems and save your budget. Otherwise, it can result in monetary losses for your clinic.
Before adopting telehealth, you should find a trusted technology vendor. Rely on our guide to choosing the right solution to make the best choice.
#4 Develop an etiquette checklist for your web-side manner
Visualize the visit from the patient’s perspective and create a professional telehealth look and feel. For example, the clothing you wear on camera might look different from what you wear during in-person meetings. When it comes to colors, the most appropriate color palette for video consulting is earth tones (also referred to as natural colors), such as deep blues, greens, and purples. Wear appropriate clothes (as you would dress for an in-person visit). Typically, that’s a lab coat with a visible name badge.
Look at some best practices for excellent web-side manner before, during, and after the visit:
Before the visit:
- Set your working hours in an automated scheduler using telehealth software so patients can see available time slots and schedule a visit with minimum back-and-forth communication.
- Get the patient’s consent to participate in the virtual visit.
- Get the patient’s details up front via a digital intake form to effectively prepare for your consultation and devote more time to addressing the patient’s needs.
- Check your connection and test your internet speed.
- Prepare your workspace. Ensure your room is private and away from distractions.
- Set up your workplace (camera at eye height, head fully within camera view so the patient can see your full face, etc.).
- Find an uncluttered background.
During the visit:
- Discuss the appointment objectives and let your patient know what to expect.
- Share instructions on what the patient should do if connectivity is lost. You may get the patient’s phone number to continue the visit over the phone or reschedule the appointment.
- Verbalize your actions to make patients feel more comfortable, such as when you’re doing something offscreen.
- Speak clearly and with appropriate brief pauses.
- Maintain eye contact, follow a proper dress code, and minimize body movements.
- Invite the patient to end the conversation, clarifying whether they have any questions, concerns, or wishes.
Post-visit:
- Provide the patient with an after-visit summary and agree on further steps. After the consultation, the patient should clearly understand what to do next.

#5 Prepare your patients for telehealth
Lots of patients are still getting used to telehealth visits. Healthcare providers should ease this transition and make patients feel confident about virtual consultations. Preparing your patients for telehealth ensures quality care and patient comfort. It eliminates patients’ fears of losing connection with doctors, uncertainty about receiving high-quality medical assistance, and doubts about access issues. Look at some actions providers should take to address behavioral barriers and make patients feel more comfortable during virtual care:
1. Choose the proper means to promote telehealth
Healthcare providers should inform patients that they provide telehealth in various ways. Telehealth promotion allows clinicians to educate their patients about available telehealth options. Providers can do this by sending emails to patients, communicating on social media, live streaming, updating information on their website, sharing information on medical portals and public groups, and so on.
2. Help your patients use telehealth technology
Many patients might experience technological barriers to adopting telehealth and not have the skills to use telehealth software. Telehealth providers should offer clear step-by-step instructions to their patients and make these instructions available in multiple languages. Let’s look at some other helpful tips for onboarding your patients while introducing telehealth:
- Ensure a telehealth assistant (coordinator, nurse) will support the patient at each stage to help ease patient frustration and reduce fears. Also, consider people’s cultural and religious backgrounds as well as language limitations when providing telehealth services.
- Discuss security and privacy issues with your patients before telehealth appointments. Apart from HIPAA, some states may have extra requirements. You should be aware of them and ask your patients to let you know if they plan to have a session with you in other state.
- Review potential technology issues and conduct an extra session to check whether the chosen technology works appropriately for you and your patient. Also, develop a solid plan if you have to deal with technical problems.
3. Obtain informed patient consent
Many telehealth platforms include electronic informed consent forms — documents that prove patients’ consent for a telehealth visit. Although each state has different laws and guidelines regarding telehealth documentation, healthcare practitioners should consider some universal rules regardless of the state of operation.
- Explain to patients their rights and possible expectations for remote appointments.
- Let patients know that it’s up to them to accept, terminate, or refuse telehealth treatment.
- Check whether patients are aware of their responsibilities during telehealth consultations (such as maintaining privacy on their side).
Patients might also fear that their personal information will be disclosed. Hence providers must ensure patients that they won’t record a virtual visit without their consent.
Learn how else patients can benefit from telehealth solutions.
#6 Train your staff
Telehealth education for medical staff is crucial to a successful telehealth rollout since insufficient knowledge of how to use new software can prevent your organization from amplifying its benefits. You can follow these tips to effectively train your teams.
- Ask your telehealth provider for medical staff training, live sessions, and other support resources (most telehealth vendors offer it as part of their services).
- Select a training method that is convenient for your team. It can be a webinar, a demo session, or a practical lesson. Such training should help participants understand how to connect with the telehealth system, features of the telehealth solution, how to use the equipment and software, and the process flow. Gather feedback after training to discover pain points and challenges. This will help you plan further educational steps.
- Run pilot sessions to help your team gain practical skills and prepare for potential challenges. Test the platform with a particular patient group and identity concerns patients might experience, such as poor connectivity, scheduling issues, poor video and/or audio quality, or billing matters.
- Define the means to understand how your program went. After each telehealth session, insert feedback loops (questionnaires, surveys, email campaigns, etc.) to find gaps, improve the system’s usability, and check whether patients have reached their goals. You can also include a 1- to 5-star rating system to better measure patient satisfaction.
- Evaluate knowledge gained during training by asking your personnel to demonstrate their skills. For example, you can prepare tests to assess educational outcomes.
Dive deep into seven effective strategies to train your staff on using telehealth to increase the success of telehealth implementation and prevent potential adoption issues.
#7 Measure success
Once your clinic implements a telehealth service, monitor the key performance indicators (KPIs) on a regular basis to measure performance and ensure it brings desired outcomes. Among the most important indicators are:
- Performance of the telehealth technology: audio and video quality, connectivity speed, number of interrupted videos and calls, etc.
- Telehealth revenue and reimbursement: the overall volume of virtual visits compared to in-person visits in the same period in prior years
- Physicians’ and patients’ satisfaction: whether patients and providers would recommend telehealth services to their friends and colleagues and continue using telemedicine in the future
To summarize
Your clinic would be halfway to successfully implementing telehealth by following these best practices. Good preparation and awareness of all the benefits, challenges, and tips for setting up and using telehealth remain key to success.
Ready to get started on implementing telehealth in your facility? Check out our latest guide to learn how to effectively plan and integrate remote healthcare solutions, provide equal access to medical care, increase business revenue, and improve patient satisfaction.
FAQ
-
- Assess the needs of new and existing patients
- Ensure privacy
- Select a telehealth vendor
- Develop an etiquette checklist for your web-side manner
- Prepare your patients for telehealth
- Train your staff
- Measure your success




